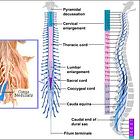
When you think joint hypermobility, don't forget about the spine
The spine has over 100 joints supported by even more ligaments. With ligament laxity, in EDS and HSD, it's no surprise that the spinal instability occurs!
Joint hypermobility is characterized by an increased range of motion beyond what is considered normal. This is sometimes reffered to as being “double jointed”. While hypermobility can be a benign trait, it is also commonly associated with connective tissue disorders such as Ehlers-Danlos Syndrome (EDS) and Hypermobile Spectrum Disorders (HSD), when it occurs throughout the body (generalized joint hypermobility) and is accompanied by other symptoms and comorbidities. EDS and HSD are conditions that result from genetic changes impacting collagen and other connective tissue proteins.
Spinal instability is a concern in individuals with EDS and HSD due to the laxity of ligaments and connective tissues supporting the spine. Instability can manifest in various ways, such as vertebral subluxations, abnormal curvature of the spine, and increased susceptibility to brainstem and spinal cord compression and neurological manifestations. Understanding and addressing spinal instability is important in these conditions to prevent complications such as chronic pain, neurological deficits, impaired mobility and poor quality of life.
Hypermobility vs. Instability
As mentioned above, hypermobility is characterized by an unusually large range of motion in one's joints, allowing them to extend, flex, or rotate beyond the normal limits. This can happen in any joints in the body and factors such as age, muscle tone and sex can influence the degree of hypermobility. It's important to differentiate between hypermobility as a benign trait and as a pathological condition. While hypermobility itself may not always cause issues or symptoms, it can predispose individuals to joint instability, especially with certain lifestyle factors and underlying conditions like EDS or HSD.
It’s crucial to note that not all hypermobility is indicative of instability. Some individuals may exhibit hypermobility without experiencing joint instability or any pain or related symptoms. Conversely, instability can occur in individuals who do not exhibit hypermobility, particularly as a result of trauma, degenerative changes, or other underlying conditions affecting the ligaments and supportive structures of the joints.
Spinal Instability
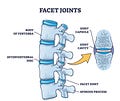
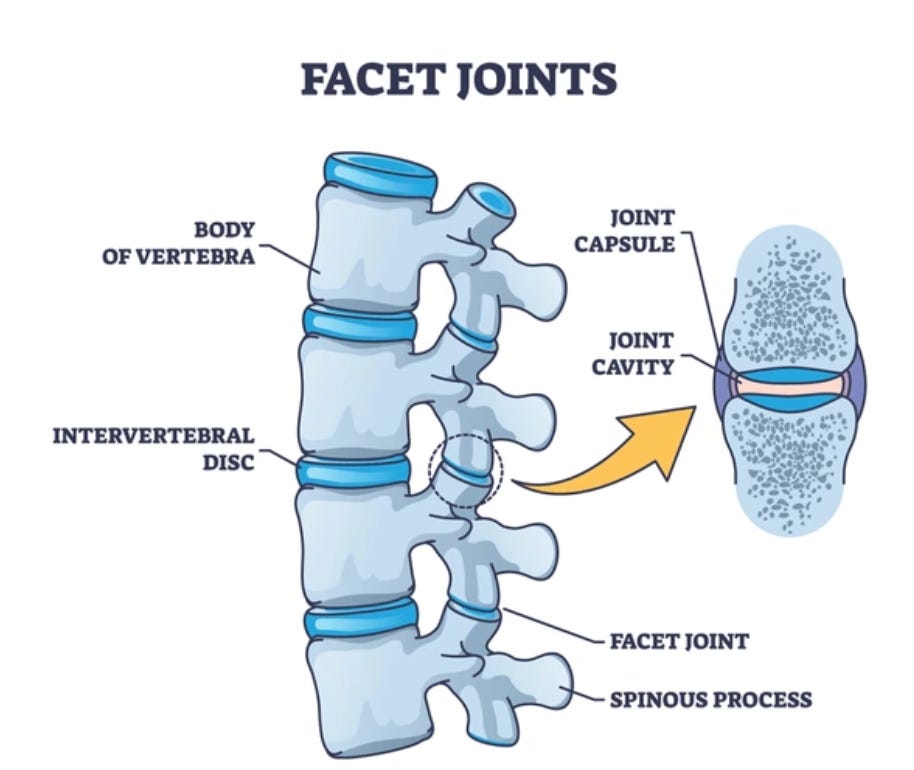
The spine is composed of multiple vertebrae stacked on top of each other, with intervertebral discs providing cushioning and flexibility. It includes over 100 joints, including facet joints that connect adjacent vertebrae, as well as numerous ligaments that provide stability and support (makes sense that ligament laxity could impact the spine!)
Upper Cervical Instability
Instability in the upper cervical spine presents unique challenges and risks due to the role of supporting the head. Conditions such as atlantoaxial instability (AAI) and cranio-cervical instability (CCI) can result from ligament laxity and structural abnormalities, leading to instability in the upper cervical spine. AAI involves excessive movement between the atlas (C1) and axis (C2) vertebrae, while CCI encompasses instability between the skull and the upper cervical spine. The potential symptoms and complications of upper cervical instability can be severe and debilitating. Individuals may experience chronic neck pain, and headaches. Moreover, instability in this region can lead to neurological symptoms such as vertigo, dizziness, and sensory disturbances, as well as more serious complications like spinal cord compression and brainstem dysfunction.
The Rest of the Spine
Spinal instability can also occur in the thoracic or lumbar regions, causing spondylolisthesis and degenerative disc disease. Instability throughout the spine can result in chronic back pain, postural abnormalities, weakness and reduced mobility. It can also exacerbate neurological symptoms and complications, such as radiculopathy and spinal cord compressionspinal. Keeping in mind that lower back pain and pain in the thoracic spine can also be due to conditions like slipping rib syndrome or tethered cord syndrome. It is important to have a comprehensive exam and imaging to pinpoint the causes of these symptoms.
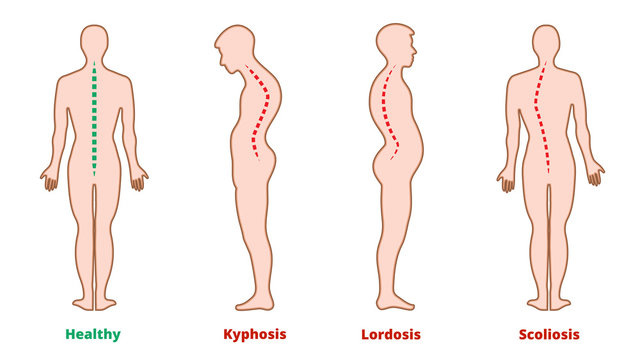
Scoliosis and Kyphosis
Individuals with EDS and HSD often face challenges related to spinal deformities such as scoliosis and kyphosis. Scoliosis is characterized by abnormal lateral curvature of the spine, while kyphosis involves an exaggerated forward curvature of the thoracic spine. These deformities can significantly impact spinal stability, posture, and function in affected individuals. Kyphoscoliotic Ehlers-Danlos Syndrome (kEDS) is a very rare subtype of EDS characterized by the presence of both kyphosis and scoliosis, along with other connective tissue abnormalities and instability.
Utility of Dynamic Imaging
Dynamic imaging techniques are important in diagnosing and evaluating spinal instability/ Unlike static imaging modalities such as conventional X-rays and MRI scans, which capture the spine in a fixed position, dynamic imaging allows healthcare providers to assess spinal mobility and stability under various conditions.
One of the primary dynamic imaging approaches used in the evaluation of spinal instability is flexion-extension X-rays. These X-rays are taken while the patient actively flexes and extends their spine, allowing healthcare providers to observe changes in spinal alignment and movement. However, X-rays do not provide detailed imaging of the brain, brainstem and spinal cord. Upright, dynamic MRI scans, which capture real-time images of the spine in flexion and extension have become the standard tool for diagnosing CCI an AAI. To learn more, check out Operation Upright by Sydney Severance.
Managing and Treating Spinal Instability
Managing and treating spinal instability involves a multifaceted approach aimed at addressing symptoms, improving stability, and enhancing overall quality of life for affected individuals. Treatment options may vary depending on the severity of spinal instability. One treatment is spinal fusion surgery, which aims to stabilize the spine by fusing two or more vertebrae together. While spinal fusion surgery can provide significant relief for some individuals, it is not without challenges and limitations. Patients with EDS are more likely to experience complications such as delayed wound healing, hardware failure, and the need for revision surgeries or additional fusions due to their inherent ligament laxity and tissue fragility. Surgical interventions for spinal instability in individuals with EDS must be carefully considered, with a thorough assessment of potential risks and benefits.
In addition to surgical interventions, conservative treatment approaches such as physical therapy may play a crucial role in managing spinal instability and associated symptoms, delaying or preventing surgery alltogether. However, it's important to recognize that managing spinal instability in individuals with EDS and HSD requires a comprehensive approach that addresses not only the spine but also other areas of the body affected by ligament laxity and connective tissue abnormalities. It is important to work with providers who have experience working with EDS patients and instability.
Comprehensive management strategies for individuals with EDS and HSD should include regular physcial therapy, management of comorbidities, and coordinated care from a multidisciplinary team of healthcare providers - yes I know, this is NOT easy to accomplish or find as a patient! Ultimately, managing spinal instability in individuals with EDS and HSD requires a personalized approach that takes into account the complex interplay of factors contributing to the condition and aims to optimize long-term outcomes and quality of life.
Some relevant blog posts to these topics can be found below:
If you enjoy this content, want access to paid subscriber exclusives or just want to support this blog, consider becoming a subscriber today!