Understanding Autonomic Dysfunction
Diving in to dysautonomia, the overlap with other conditions, and the latest in research
In this blog post, we’ll delve deeper into the world of dysautonomia, explaining what dysautonomia is, how dysautonomia intersects with conditions like Ehlers-Danlos syndrome (EDS), viral infections, and small fiber neuropathy, and discuss the lastest research.
The Autonomic Nervous System
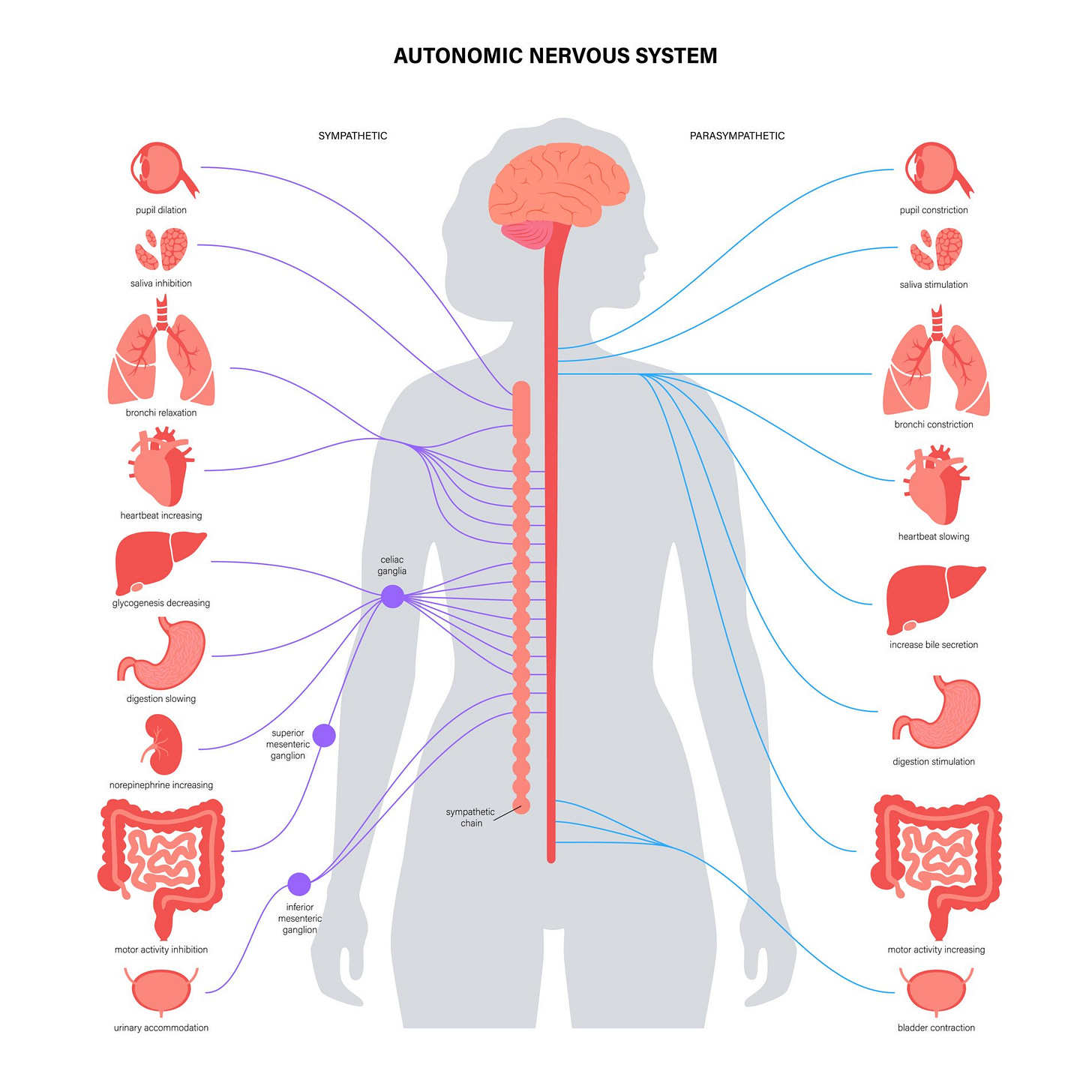
The Autonomic Nervous System (ANS) is the part of your nervous system that controls automatic body functions. The ANS is made up of the sympathetic and parasympathetic systems that control involuntary functions, such as heart rate, blood pressure, digestion, and temperature. The sympathetic nervous system is responsible for the “flight or flight” response, while the parasympathetic nervous system is responsible for what is commonly called “rest and digest” processes. The ANS includes nerves in the brain, spinal cord, and throughout the body that reach limbs and organs.
Dysautonomia
Dys” means abnormal or impaired, and “autonomia” refers to the autonomic nervous system. Dysautonomia refers to a group of conditions where the ANS doesn't function properly. This dysfunction can lead to a wide range of symptoms and can significantly impact quality of life. Symptoms can include but are not limited to: dizziness and fainting, rapid heart rate, fatigue, and gastrointestinal dysfunction.
Types of Autonomic Dysfunction
Some types of dysautonomia include*:
POTS (Postural Orthostatic Tachycardia Syndrome) - Most common
POTS causes symptoms when someone goes lying down to being upright (postural). Symptoms commonly include a fast heart rate, dizziness and fatigue but can also include additional manifestations.
Inappropriate Sinus Tachycardia (IST)
IST is a heart rhythm disorder that causes a very fast heart rate, palpitations, weakness, chest pain, shortness of breath fatigue and dizziness.
Neurocardiogenic Syncope, also referred to as Vasovagal Syncope
Neurocardiogenic or vasovagal syncope causes a drop in blood pressure that may also affect heart rate, causing dizziness, pre-syncope or fainting, caused by some sort of trigger.
Multiple System Atrophy (MSA)
MSA involved widespread autonomic nerve damage that can present similarly to Parkinson’s disease. Symptoms can be progressive that begin with orthostatic hypotension, pupil dilation, loss of bladder function, sleep apnea, and trouble eating, swallowing and speaking
Pure Autonomic Failure (PAF)
PAF is a degenerative condition that develops in adulthood mainly causing orthostatic hypotension, changes in sweat production, inappropriate pupil dilation, bladder and bowel dysfunction, and sexual dysfunction.
It is estimated that 70 million people worldwide have dysautonomia. POTS is relatively common and tends to be more prevalent in young women, though it can impact any age and gender. Other types of dysautonomia however, are more rare.
*There are additional types of Dysautonomia not included above, but for the sake of space I have chosen to leave them out of this article.
Comorbidities and Overlapping Conditions
Dysautonomia often doesn’t occur in isolation. It may overlap or co-occur with other health conditions, complicating diagnosis and treatment. Sometimes, there may be a cause-and-effect relationship. In other cases, the relationship is not as clear. Understanding these intersections is important for effective management.
Ehlers-Danlos Syndromes
The Ehlers-Danlos Syndromes (EDS) are a group of connective tissue disorders that are often seen alongside dysautonomia, particularly Postural Orthostatic Tachycardia Syndrome (POTS). A recent study revealed that 70% of people with hypermobile EDS (hEDS) report also having a diagnosis of POTS.
It has been suggested that the connective tissue abnormalities in EDS can lead to issues with blood vessel structure and function, contributing to autonomic dysfunction. However, the exact relationship between EDS and POTS requires further research to understand the underlying mechanisms at play.
Viral Infections
Viral infections and immune triggers, such as Epstein-Barr virus and COVID-19 can trigger or worsen dysautonomia. In some cases, individuals develop dysautonomia after recovering from a viral illness. Dysautonomia/POTS is often associated with ME/CFS and long COVID. The exact mechanism of post–COVID–19 POTS is unknown but likely involves an autoimmune component.
Small fiber Neuropathy
Small fiber neuropathy involves damage to the small nerve fibers that help regulate autonomic functions. This nerve damage can lead to or exacerbate autonomic dysfunction and may be present in up to 50% of people with POTS. Small fiber neuropathy can cause neuropathic symptoms such as burning nerve pain, impaired temperature sensation, a pins and needles sensation, and numbness. Small fiber neuropathy has also been reported in patients with EDS.
Other Overlapping Conditions
Dysautonomia can coexist with other conditions too, such as:
Autoimmune diseases
Mast cell activation diseases
Diabetes
Multiple sclerosis
Chiari malformation
Mitochondrial diseases
Parkinson's disease
Charcot Marie Tooth disease
& more
Dysautonomia Research
Ongoing research is crucial for uncovering the underlying mechanisms that lead to autonomic dysfunction. By understanding the biological mechanisms behind dysautonomia, we can develop more effective treatments and improve the quality of life for those affected.
Pathophysiological Mechanisms
The pathophysiology of POTS is an important area of research. Some mechanisms include:
Increased sympathetic activity and circulating catecholamines (hyperadrenergic POTS)
Lower blood volume (hypovolemic POTS)
Reduced cardiac stroke volume and mass, can be due to bed rest (deconditioning)
Autoimmunity
Peripheral sympathetic nerve damage and increased compensatory heart rate (small fiber neuropathy, also referred to as neuropathic POTS)
The Role of Genetics
While no single genetic cause has been identified for POTS, there is evidence of a genetic component. Family studies have shown that POTS patients may have family members with the condition or with joint hypermobility and autoimmune diseases. Some specific genetic associations are currently being researched to understand how they may be related to POTS. One variant that has been identified, in GNB3, was found to be more common in POTS patients and linked to an increase in heart rate upon standing. Additional SNPs have been identified in NOS3 in patients with POTS. Both of these discoveries may play a role in the development or progression of POTS, but have not been shown to be causative of the condition. Other types of dysautonomia, such as familial dysautonomia, do have definitive genetic causes that can be identified by genetic testing.
Environmental and Immune Triggers
Clinical data suggest that POTS often follows viral infections, pointing to a possible immunological trigger. Positive autoantibody tests are common among POTS patients. Some recent studies have looked at specific autoantibodies targeting cardiovascular G-protein coupled receptors (α1‐, β1‐ and β2‐adrenergic receptors), ganglionic acetylcholine receptor (gAChR), and cardiac lipid raft‐associated proteins. Stressful events and physical trauma are known triggers for autonomic dysfunction, however the exact mechanism requires further research.
Promising Areas of Research
Some emerging areas of research include:
Autoantibodies as a cause of POTS (see linked publications above)
Intravenous immunoglobulin (IVIG) and plasmapheresis as a treatment for POTS
Vagus Nerve Stimulation as a treatment
Biomarker Studies
Low Dose Naltrexone as a treatment
Mitochondrial dysfunction
Neuro-immune-GI relationships
Some funded studies through Dysautonomia International on POTS, dysautonomia and Long COVID are also underway. You can also check out Clinical rials.gov studies and NIH Funded research grants.
Whether you’re newly diagnosed, supporting a loved one, or simply looking to expand your understanding, I hope this provided a helpful overview with lots of resources to learn more. To see the corresponding Instagram post series with graphics and share them, head to my instagram here!
Resources to learn more:
References:
Vernino S, Bourne KM, Stiles LE, et al. Postural orthostatic tachycardia syndrome (POTS): State of the science and clinical care from a 2019 National Institutes of Health Expert Consensus Meeting - Part 1. Auton Neurosci. 2021;235:102828. doi:10.1016/j.autneu.2021.102828
Petrucci T, Barclay SJ, Gensemer C, Morningstar J, Daylor V, Byerly K, Bistran E, Griggs M, Elliot JM, Kelechi T, Phillips S, Nichols M, Shapiro S, Patel S, Bouatia-Naji N, Norris RA. Phenotypic Clusters and Multimorbidity in Hypermobile Ehlers-Danlos Syndrome. Mayo Clin Proc Innov Qual Outcomes. 2024 May 15;8(3):253-262. doi: 10.1016/j.mayocpiqo.2024.04.001. PMID: 38779137; PMCID: PMC11109295.
Nakao R, Tanaka H, Takitani K, Kajiura M, Okamoto N, Kanbara Y, Tamai H. GNB3 C825T polymorphism is associated with postural tachycardia syndrome in children. Pediatr Int. 2012 Dec;54(6):829-37. doi: 10.1111/j.1442-200X.2012.03707.x. Epub 2012 Nov 21. Erratum in: Pediatr Int. 2013 Jun;55(3):399. PMID: 22882749.
Garland EM, Winker R, Williams SM, Jiang L, Stanton K, Byrne DW, Biaggioni I, Cascorbi I, Phillips JA 3rd, Harris PA, Rüdiger H, Robertson D. Endothelial NO synthase polymorphisms and postural tachycardia syndrome. Hypertension. 2005 Nov;46(5):1103-10. doi: 10.1161/01.HYP.0000185462.08685.da. Epub 2005 Oct 3. PMID: 16203873.
El-Rhermoul FZ, Fedorowski A, Eardley P, Taraborrelli P, Panagopoulos D, Sutton R, Lim PB, Dani M. Autoimmunity in Long Covid and POTS. Oxf Open Immunol. 2023 Mar 8;4(1):iqad002. doi: 10.1093/oxfimm/iqad002. PMID: 37255928; PMCID: PMC10224806.
Igharo D, Thiel JC, Rolke R, et al. Skin biopsy reveals generalized small fibre neuropathy in hypermobile Ehlers-Danlos syndromes. Eur J Neurol. 2023;30(3):719-728. doi:10.1111/ene.15649
Watari M, Nakane S, Mukaino A, Nakajima M, Mori Y, Maeda Y, Masuda T, Takamatsu K, Kouzaki Y, Higuchi O, Matsuo H, Ando Y. Autoimmune postural orthostatic tachycardia syndrome. Ann Clin Transl Neurol. 2018 Feb 28;5(4):486-492. doi: 10.1002/acn3.524. PMID: 29687025; PMCID: PMC5899914.
Li H, Yu X, Liles C, et al. Autoimmune basis for postural tachycardia syndrome. J Am Heart Assoc. 2014;3(1):e000755. Published 2014 Feb 26. doi:10.1161/JAHA.113.000755